Revisiting Bisphosphonates and Femur Fractures
Nearly six years ago in this column, I discussed what was then a little-known problem associated with long-term use of bisphosphonates, the valuable drugs that protect against fractures caused by bone loss. The drugs, among them Fosamax, Actonel and Boniva, can slow bone loss, increase bone density and cut fracture rates in half in women with established osteoporosis.
Reports had begun to emerge that some women taking bisphosphonates for many years suffered an unusual fracture of the femur, the long bone of the thigh. There was little or no trauma; in most cases the women were simply standing or walking when the femur snapped in half. In some, breaks occurred in both thighs, and many of the fractures were unusually slow to heal.
Experts think the fractures happened because of the way the drugs work: by slowing the rate of bone remodeling, the normal process by which injured bone heals. As a result, microfractures that occur through normal wear and tear are not repaired. Although bone density may be normal, the bone can become brittle and crack under minor stress.
In the years since, hundreds of cases of atypical femur fractures have been reported among women and some men taking bisphosphonates for five or more years. A number of studies have tried to assess the risk, and last fall the Food and Drug Administration issued a “safety announcement” and required that the drugs’ labels warn physicians and patients to be alert for this potential complication.
So, with all of the problems associated with these drugs and the realized benefit, do the risks outweigh the benefits? The latest study was published in JAMA on February 23rd.
“Compared to the number of fractures prevented,” she said, “the actual risk of a subtrochanteric femur fracture is small” — 1 case in 1,000 in the sixth year of therapy and 2.2 cases in 1,000 the seventh year.
And, in another report in the The New England Journal of Medicine.
A report published last year in The New England Journal of Medicine found no increase in atypical femur fractures, but that study did not include enough patients taking bisphosphonates for many years to produce a reliable result. Preliminary data from a much larger study has indicated that the risk of atypical femur fractures increased from 2 cases a year per 100,000 users after two years of bisphosphonate therapy to 78 cases a year per 100,000 after eight years on the drug.
In a report from a 27-member task force of the American Society for Bone and Mineral Research (published online in September in The Journal of Bone and Mineral Research), the experts noted that the way bisphosphonates work can reduce the “toughness” of bones. “It is highly likely that case reports and case series of atypical femur fractures will continue to accumulate,” the task force wrote, noting that another 47 cases had been reported since their analysis was prepared. Many cases are not reported, and in an unknown number of cases physicians may not recognize the fractures as atypical.
The task force called for an international registry of cases, including details that could help define who is most at risk.
So, what should a patient and a dentist do?
Certainly, be aware of the inherent risks of the bisphosphonates and be sensitive to the need, particularly if you are not at a high fracture risk.
Initial excitement about bone-protecting drugs led to prescriptions for millions of women who were not necessarily at high fracture risk, and many experts now urge a thorough evaluation before a bisphosphonate is prescribed. In addition to bone density test results, the evaluation should take into account a patient’s smoking and drinking habits, thinness, family history of osteoporosis, previous osteoporotic fractures, drug prescriptions and weight-bearing exercise regimen. An online evaluation tool developed by the World Health Organization is at www.shef.ac.uk/FRAX, though some experts have criticized it as incomplete.
The task force said a decision to treat should be “based on an assessment of benefits and risks,” and added, “patients who are deemed to be at low risk of osteoporotic-related fractures should not be started on bisphosphonates.”
Even those with osteoporosis in the spine but little or no problem in their hips, the experts concluded, should consider alternative remedies.
Osteonecrosis of the jaw is NOT a minor complication and the dentist in consult with the patient and patient’s physician must evaluate the risks, prior to dental surgery.
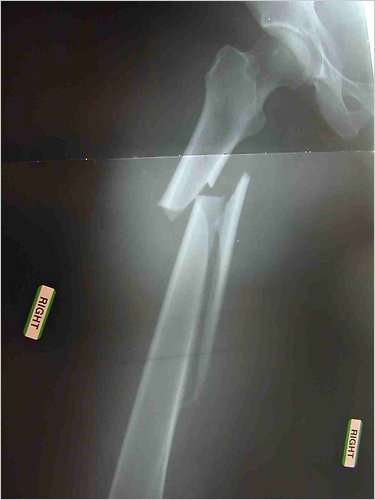
The femur of Dr. Jennifer Schneider of Tucson, an internist who after seven years on Fosamax suffered a nontraumatic femur fracture that took two years to heal
Dr. Schneider invites patients who have had such a fracture to write her at jennifer@jenniferschneider.com
Previous:
New Dentistry Cause for Alarm for Patients Who Use Bisphosphonates – Fosamax, Actonel, Boniva?
3 Comments
Pingback:
Pingback:
Pingback: